Die Behandlung von Narben kann nach einer Brandverletzung unangenehm sein. In der Schwabinger Klinik sollen nun virtuelle Unterwasserwelten junge Patienten ablenken.
Wenn Carsten Krohn seine Patientinnen und Patienten behandelt, hört er nicht selten, wie sie plötzlich aufschreien: Er leitet das „Zentrum für schwerbrandverletzte Kinder“ an der München Klinik(Mük) Schwabing und muss häufig die Narben der Kinder behandeln, damit das Gewebe flach und elastisch bleibt – und das kann für sie schmerzhaft sein.
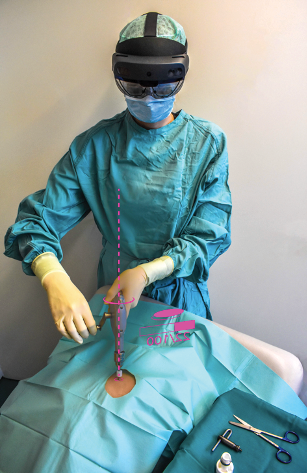
Neuerdings könnten im Behandlungszimmer aber immer öfter keine Schmerzens-, sondern Freudenschreie erklingen: Die kleinen Patientinnen und Patienten dürfen nämlich in eine wundersame Meereswelt eintauchen, mit Delfinen und Oktopussen. Das ermöglicht ihnen eine VR-Brille. VR steht für virtuelle Realität, eine computergenerierte Umgebung, in die ein Mensch quasi eintauchen kann – wenn er oder sie eine spezielle Brille aufsetzt.
Seit vergangenem Sommer sind die Brillen in der Klinik im Einsatz. Die Mük Schwabing hat sie mithilfe einer Spende des Rotary Clubs München-Hofgarten für vier Jahre angeschafft, um den Kindern dabei zu helfen, die Narbenbehandlungen nach Brandverletzungen besser auszuhalten. „Sie sind durch die visuelle Ablenkung entspannter und kooperativer und geben weniger Schmerzen an. Das ist eine große Hilfe, sowohl für die Kinder als auch für uns als Behandler, und es ist auch für die Eltern stressfreier“, sagt Krohn, der auch der leitende Oberarzt in der Schwabinger Kinderchirurgie ist.
Auch vergehe die Behandlungszeit für die Patientinnen und Patienten durch den Einsatz der VR-Brillen subjektiv schneller. Zudem könne die Gabe von Schmerz- und Narkosemitteln reduziert werden – ein noch größerer Erfolg für alle. Die Behandlung der Narben nach Verbrennungen durch Spezialistinnen und Spezialisten ist laut Krohn essenziell, um ein funktionell und optisch gutes Ergebnis zu erzielen und das Leid der Betroffenen zu mindern. Denn jede Narbe sei eine Last, besonders an sichtbaren Körperpartien. Jährlich behandelt das „Zentrum für schwerbrandverletzte Kinder“ der Mük mehr als 150 Kinder, 70 Prozent von ihnen haben mit Verbrühungen erlitten.
Ein bis zwei Kinder pro Tag kommen in den Genuss der Meereswelt in der VR-Brille, berichtet Krohn. Etwa ab dem Schulalter funktioniere sie seiner Erfahrung nach gut, denn die Kinder müssten sich auf das Abenteuer einlassen können. Auch eine Interaktion zwischen den anwesenden Ärztinnen und Pflegerinnen, den Eltern und den Kindern sei wichtig. Denn die Kinder kämen ins Erzählen darüber, was sie gerade sehen, und man sollte darauf eingehen, um sie für die Dauer der Behandlung weiter in der virtuellen Welt zu halten.
Mittlerweile werden die VR-Brillen auch in der Kinder-Physiotherapie eingesetzt, so die Mük. Auch in anderen Fachabteilungen könne man sich den Einsatz gut vorstellen. Studien belegten die schmerzlindernde Wirkung bei akutem Schmerzerleben durch VR-Brillen. Doch es gibt noch viel zu verstehen: Die genauen neurophysiologischen Mechanismen, die dabei im Gehirn ablaufen, seien komplex und bisher nicht genau bekannt.
Quelle:
Foto: Mithilfe der VR-Brille können die Kinder während der Behandlung in Meereswelten abtauchen.(Foto: München Klinik)
https://www.sueddeutsche.de/muenchen/muenchen-klinik-schwabing-medizin-kinder-vr-brille-1.6519045